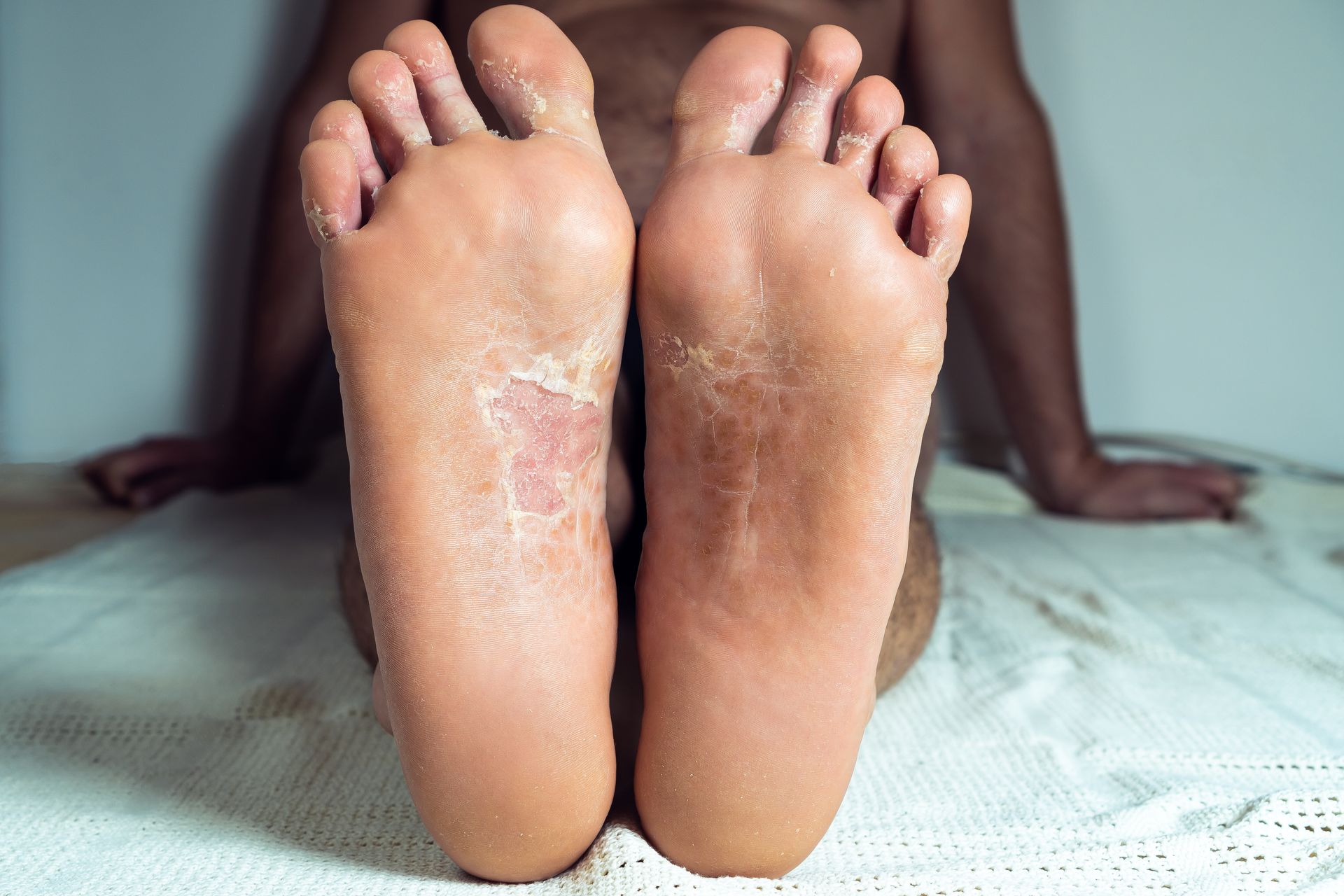
Neuropathy symptoms in feet to watch
Neuropathy symptoms in your feet can start subtly—then gradually interfere with sleep, balance, and everyday comfort. If you have diabetes, a history of nerve issues, frequent foot injuries, or you’re simply noticing “weird” sensations that weren’t there before, it’s worth paying attention. These warning signs matter because reduced sensation can make it easier to miss blisters, cuts, pressure points, or infections until they become more complicated to treat. As spring routines pick up and you’re on your feet more, small changes can be easier to overlook. The goal isn’t to panic—it’s to recognize patterns early, protect your skin, and know when it’s time to get a professional opinion.
Bottom Line Upfront: Key Warning Signs
- Numbness or reduced feeling in toes/soles can make injuries easier to miss.
- Tingling, “pins and needles,” or burning sensations that persist or worsen deserve attention.
- Nighttime foot pain or sensitivity (even to sheets) can signal nerve irritation.
- Balance changes or feeling “unstable” may be linked to altered sensation in the feet.
- New sores, blisters, or skin breakdown —especially if you didn’t feel them happen—should be checked promptly.
- Color/temperature changes in the feet can be a sign to get evaluated, particularly if one foot differs from the other.
How Foot Nerve Symptoms Typically Show Up
Peripheral neuropathy involves irritation or damage to nerves that carry sensation (and sometimes motor signals) between your feet and your brain. In the feet, this often shows up in a “stocking-like” pattern—starting at the toes and moving upward over time. Symptoms can be sensory (numbness, burning, tingling), pain-related (sharp, electric, or aching discomfort), or functional (balance issues, clumsiness, weakness).
Not every odd sensation equals neuropathy, and symptoms can overlap with circulation problems, skin conditions, back issues, or footwear-related pressure. That’s why the trend over time matters: what you feel, how often it happens, whether it’s spreading, and whether it affects your ability to walk comfortably or notice injuries.
Why These Signs Matter If You Wait
When nerve sensation is reduced, you may not feel friction, heat, or pressure the same way. Practically, that can lead to:
- Delayed discovery of wounds: a blister can become an open sore before you realize it’s there.
- Higher infection risk: even small breaks in skin can worsen if not cleaned, protected, and monitored.
- More falls or ankle sprains: decreased feedback from the feet can affect balance and reaction time.
- Sleep disruption and fatigue: burning or electric sensations often feel worse at night for some people.
- More trial-and-error spending: repeated shoe inserts, creams, or gadgets can add up if the root cause isn’t identified.
Early evaluation doesn’t guarantee a specific outcome, but it can help you understand what’s driving the symptoms and what protective steps make the most sense for your feet.
Common Missteps That Can Make Foot Nerve Issues Worse (Checklist)
- Ignoring numbness because it “doesn’t hurt”: lack of pain can still mean higher risk of unnoticed injury.
- Soaking feet in very hot water: reduced sensation can make burns more likely—test water with your elbow or a thermometer.
- Walking barefoot at home: tiny cuts, splinters, and stubbed toes are easier to miss.
- Using sharp tools on calluses or corners of nails: small nicks can become bigger problems if healing is slow.
- “Toughing it out” with painful shoes: pressure points can create blisters and skin breakdown quickly.
- Self-treating a wound with harsh chemicals: some antiseptics can irritate tissue—when in doubt, use gentle cleansing and get guidance.
A Smart Action Plan If You Notice Changes (Checklist)
- Do a daily foot check: look at toes, soles, heels, and between toes; use a mirror or ask for help if needed.
- Track symptoms for 1–2 weeks: note when they happen (night vs. day), what they feel like, and whether they’re spreading.
- Protect your skin: keep feet clean and dry, moisturize tops and bottoms (avoid lotion between toes), and change socks daily.
- Choose footwear that reduces friction: wide toe box, supportive sole, no internal seams rubbing; break in new shoes gradually.
- Address small problems early: cover hot spots, pad pressure areas, and stop the activity/shoe that caused irritation.
- Manage health factors you can control: follow your care plan for blood sugar (if applicable), nutrition, and activity; discuss medication side effects with your prescribing clinician.
Professional Insight: What Most People Miss Early On
In practice, we often see people focus on the sensation itself (tingling, burning, numbness) and miss the second-order issue: skin protection. The feet can look “fine” until one day there’s a blister from a new shoe, a crack in the heel, or a sore spot that didn’t hurt—then it suddenly becomes urgent. Treating symptoms and protecting the foot at the same time is usually a smarter, calmer approach than waiting for a visible problem to force the issue.
When It’s Time to Seek Medical Help for Foot Nerve Concerns
Consider getting evaluated if you notice any of the following:
- New or worsening numbness that affects how you walk or how well you feel the ground.
- Burning, stabbing, or electric pain that persists, disrupts sleep, or keeps returning.
- A sore, blister, or cut that isn’t improving, is draining, or looks red/swollen.
- Signs of infection such as spreading redness, warmth, pus, or fever (seek urgent care as appropriate).
- Sudden weakness, foot drop, or major balance changes —especially if it comes on quickly.
- One foot looks different than the other in color, temperature, or swelling without a clear reason.
If you have diabetes or a history of foot ulcers, it’s especially important to take new foot changes seriously and get guidance sooner rather than later.
Your Questions, Answered
How can I tell if tingling in my toes is a serious issue?
If tingling is persistent, worsening, spreading, or paired with numbness, pain at night, balance changes, or skin problems, it’s a good reason to get evaluated. A clinician can help sort out whether it’s nerve-related, pressure-related, circulation-related, or something else.
Is numbness in the feet always caused by nerve problems?
No. Numbness can be associated with nerve irritation, but it can also relate to circulation concerns, back issues, footwear pressure, or other medical conditions. Because the causes vary, an exam and history are often the fastest way to narrow it down.
What should I do if I find a blister or sore I didn’t feel?
Clean it gently, protect it with an appropriate dressing, avoid the shoe or activity that caused friction, and monitor closely. If it’s large, painful, draining, looks infected, or isn’t improving, seek medical care promptly—especially if you have diabetes.
Can footwear really make nerve discomfort feel worse?
Yes. Tight toe boxes, rubbing seams, and inadequate support can increase pressure and friction, which may aggravate discomfort and raise the risk of skin breakdown—particularly if sensation is reduced.
What can I do today to reduce my risk of foot complications?
Start with daily foot checks, consistent skin care, well-fitting shoes, and early attention to hot spots or minor wounds. If symptoms are progressing or interfering with daily life, schedule an evaluation to get a clear plan.
Taking Action Without Overreacting
Foot nerve changes are easy to dismiss until they start affecting comfort, sleep, or safety. Watching for patterns—numbness, burning, tingling, balance changes, and wounds you didn’t feel—can help you act earlier and protect your feet. If something is worsening, recurring, or paired with skin breakdown, it’s reasonable to get checked. The right next step is usually a clear assessment and a practical plan you can follow.
Ready to Get Started?
Our team is here to help. Give us a call to discuss your needs.